It may be surprising to some people to learn that physical injuries can contribute to neurodegenerative diseases. In mice, traumatic brain injuries have been previously shown to induce an Alzheimer’s-like condition, complete with amyloid plaques and neuroinflammation. In a study published this week in the journal Spinal Cord, researchers from the National Taiwan University investigated whether a similar connection exists between spinal cord injuries (SCI) and Alzheimer’s disease.
The researchers utilized medical records from Taiwan’s National Health Insurance Research Database. Their analyses included 9,257 individuals with an SCI and 37,028 non-SCI individuals, with an average age of approximately 63 years. When selecting the subjects for the study, the researchers applied an algorithm that would correct for the effects of other Alzheimer’s disease risk factors, such as age, sex, and cardiovascular health.
Over the course of a three-year period, a total of 25 SCI inviduals and 57 non-SCI individuals were diagnosed with Alzheimer’s. These numbers are quite low, possible due to the difficulty in diagnosing Alzheimer’s with high certainty, since its symptoms are similar to other forms of dementia. Cumulatively, the incidence of an Alzheimer’s diagnosis during the three-year study period was 71% higher in people with a SCI compared to people without a SCI. (I want to emphasize that this does not mean SCI patients are 71% more likely to get Alzheimer’s over their entire lifetime; this number only applies to the three-year period examined in this study.)
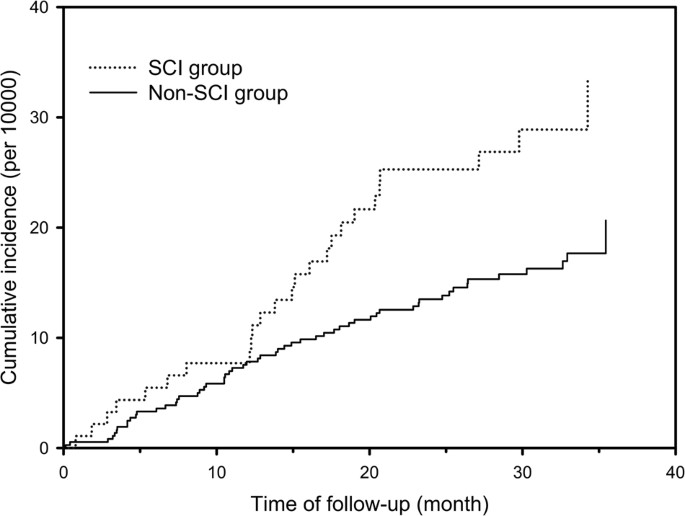
This figure from the paper shows the incidence of Alzheimer’s disease over a three-year period. The SCI individuals had an increased risk of Alzheimer’s than the non-SCI individuals.
This study is the first large-scale, longitudinal analysis to demonstrate a correlation between SCI and Alzeimer’s disease. Future research is warranted to determine what might be causing this connection. The authors suggested several possible explanations. It has been previously shown that tau and the amyloid precursor protein are deposited throughout the spinal cord following a SCI. These proteins are both closely linked to the pathogenesis of Alzheimer’s disease, so this could be a possible disease mechanism. Another possibility is that the widespread inflammation triggered by a SCI could perturb the delicate chemistry of molecules within the brain.
There are several important caveats to note with this study. For one thing, while the researchers accounted for health-related Alzheimer’s risk factors, including various medical conditions like diabetes and stroke, their records did not include information about lifestyle-related risk factors, such as smoking or exercise. These factors could have potentially skewed the analysis. Also, since the follow-up period was only three years, the data does not give us information about any longer-term effects of SCI. Finally, while the total sample size was large, only a small subset of subjects were diagnosed with Alzheimer’s, reducing the statistical power of the analysis. Future studies will need to address these problems in order to provide further insight into the emerging connection between SCI and Alzheimer’s disease.



